AMG 757 Elicits Early Response, Safety in Small Cell Lung Cancer
First-in-human results of a phase 1 trial (NCT03319940) evaluating AMG 757 in patients with small cell lung cancer revealed early signals of efficacy and a favorable safety profile in findings presented at the European Lung Cancer Virtual Congress 2021.
First-in-human results of a phase 1 trial (NCT03319940) evaluating AMG 757 in patients with small cell lung cancer revealed early signals of efficacy and a favorable safety profile in findings presented at the European Lung Cancer Virtual Congress 2021. AMG 757 is a DLL3-targeting bispecific T-cell engager.
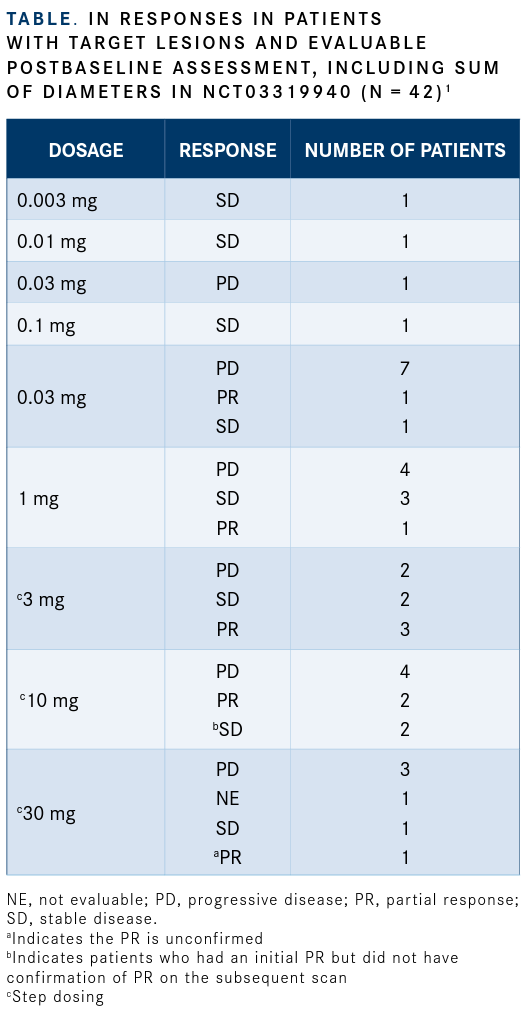
Results showed that in the 52-patient trial the agent elicited a confirmed partial response (PR) rate of 14% and an unconfirmed PR in 1 patient (TABLE1), 22% of patients had stable disease, and the disease control rate was 37%. Tumor shrinkage was observed in 40% of patients (KEY FINDINGS1).
“AMG 757 showed acceptable safety and preliminary evidence of efficacy,” Fiona H. Blackhall, PhD, FRCP, an author on the study and chair of thoracic oncology at The University of Manchester in England, said in a virtual presentation during the meeting. “The maximum dose of this compound has not been reached, dose escalation continues, and dose optimization for monotherapy is ongoing.”
AMG 757 is a novel immuno-oncology compound, defined as a half-life extended bispecific T-cell engager (BiTE) with both anti-CD3 and anti-DLL3 moieties with an Fc domain.
In the multicenter, open-label, phase 1 study, AMG 757 was delivered intravenously (IV) at doses escalating from 0.003 to 30 mg, every 2 weeks with or without step dosing. Antitumor activity was assessed using modified RECIST v1.1 criteria every 8 weeks.
The primary end points were safety, tolerability, and determination of the maximum-tolerated dose or recommended phase 2 dose. Secondary end points were pharmacokinetics and preliminary antitumor activity; exploratory objectives were to evaluate immunogenicity, biomarkers, target protein, and outcomes.
The median age was 64 years (range, 32-80) and 69% of patients were former smokers; 15% were current smokers. The majority (98%) of patients had an ECOG performance status of 0 or 1, and 75% of patients had received 1 to 2 prior lines of therapy; the median number of prior therapies was 2 (range, 1-6). Forty-four percent of patients had received a prior PD-1/ PD-L1 inhibitor. Additionally, 96% of patients had received an initial diagnosis of extensive-stage disease, 25% had brain metastases, and 48% had liver metastases.
Additional data showed that 20% have completed 24 weeks of treatment, and 4 patients with confirmed PR are still receiving treatment with an ongoing response. In patients who had a confirmed PR (n = 7), the median time to response was 1.8 months, and the estimated duration of response was greater than 6 months in 83% of patients at a median follow-up of 11.5 months.
Regarding safety, all-grade and grade 3 or higher treatment-related adverse events (TRAEs) occurred in 79% and 23% of patients, respectively. All-grade TRAEs occurring in 10% or more of patients included cytokine release syndrome (CRS; 44%; grade ≥ 3, 2%), pyrexia (19%), fatigue (14%), anemia (10%; grade ≥ 3, 2%), and nausea (10%).
Grade 4 or higher AEs occurred in 7.6% of patients and were pneumonitis (n = 1) and lymphocytopenia (n = 3); 1 patient died from pneumonitis.
The severity of CRS was typically mild, she added, and was characterized by fever (31%), tachycardia (19%), and nausea (14%). The AE was generally reversible with supportive care, steroids, IV fluids, and/or anti–IL-6 therapy, and CRS was not linked with discontinuation of treatment or deaths.
Investigators also explored the early increase in cytokine levels that were associated with the development of CRS. All cases of CRS occurred in the first cycle of treatment; 2 recurrences were reported in cycles 2 and 3. The median time to onset was 9 hours (range, 3-52) following a dose of AMG 757; the median duration of CRS was 60 hours (range, 3-197).
Additionally, there were significant increases in TNF-α, IL-10, MCP-1, IL-8, IFN-α, MIP-1β/α, and IFNγ levels from baseline in the 24 hours following the first AMG 757 dose in cycle 1 in patients who had CRS vs those who did not.
REFERENCE
1. Paz-Ares L, Owonikoko TK, Johnson M, et al. Phase 1 study of AMG 757, a delta-like ligand 3 (DLL3) targeting, half-life extended bispecific T-cell engager immuno-oncology therapy, in small cell lung cancer. J Thorac Oncol. 2021;16(4):S720-S721. doi:10.1016/S1556-0864(21)01890-6
Biomarker Testing Paves the Way for Better Targeted Therapies in NSCLC
April 16th 2024At a live virtual event, Edward S. Kim, MD, MBA, discussed the evolving landscape of biomarker testing before making treatment decisions for patients with early-stage non–small cell lung cancer (NSCLC).
Read More