Marks Explores Cardiac Toxicities and Dosing Concerns of BTK Inhibitors in CLL
During a Case-Based Roundtable® event, Stanley M. Marks, MD, moderated a discussion on the impact of cardiac adverse events on patients who receive a Bruton tyrosine kinase inhibitor for chronic lymphocytic leukemia.
Stanley M. Marks, MD (MODERATOR)
Chairman, UPMC Hillman Cancer Center
Chief, Division of Hematology/Oncology at UPMC Shadyside
Clinical Professor of Medicine, University of Pittsburgh School of Medicine
Pittsburgh, PA

EVENT REGION Pennsylvania
PARTICIPANT LIST Alexander Barsouk, MD | Jose Silva, MD | Ayodele Ayoola, MD | Rahim Remtulla, MD | Mariya Apostolova, MD
MARKS: Most would agree that acalabrutinib and zanubrutinib are both indicated as frontline therapy for chronic lymphocytic leukemia [CLL] and they both have a better safety profile than ibrutinib.1,2 But now zanubrutinib can be given once a day.3 Do you think that’s important for patients whereas acalabrutinib has to be given twice daily?4
BARSOUK: It is important, but not as much as looking at preexisting conditions and risks, [such as] whether somebody has cardiac risks or thrombocytopenia or [is] on an anticoagulant. Those considerations would override once-a-day or twice-a-day [dosing]. But with other things comparable, once-a-day [dosing] is better from an adherence standpoint.
MARKS: Cardiac events, atrial fibrillation, and atrial flutter are a class effect of all these BTK inhibitors. Evaluating the AE profiles for all 3, what impact does cardiac toxicity have on your choice of therapy?
BARSOUK: If somebody had a significant cardiac preexisting condition, I would stay away from ibrutinib. But we don’t really use ibrutinib anymore. If you [make an] indirect comparison between acalabrutinib and zanubrutinib, they’re both pretty good. There is no direct comparison…in terms of cardiac AEs and tolerance. The risks are small, but if somebody is on an anticoagulant, maybe it should be taken into consideration that patients on acalabrutinib have less risk of bleeding than on zanubrutinib if they need to be on a full-dose non–vitamin K antagonist oral anticoagulant or warfarin.
MARKS: Are you comfortable using these drugs in patients who are on direct oral anticoagulants?
BARSOUK: Yes, but you have to be careful.
SILVA: Frankly, my biggest driver for treatment is the twice-daily vs daily [dose] for most of those patients. That’s why I’ve been using more zanubrutinib in patients for whom I prescribed [medication] recently. In the past 4 or 5 cases, I started zanubrutinib for that reason specifically. It is also an easier schedule for dose reductions. For some reason, there’s a lot of fatigue associated with acalabrutinib, and because it’s [given as a] 100-mg tablet once in the morning and once in the evening, dose reductions to 50% [would be a] dose reduction to taking once a day,4 and we don’t know whether that affects the pharmacokinetics [and in turn] affects the drug’s efficacy, so I’m not very keen on that.
MARKS: Good point. The only way to dose-reduce is to give it once a day, and we don’t know. I have had patients who take it once a day. For whatever reason, they elect to, and I have seen responses, but we don’t know that it’s as effective as twice daily [dosing], whereas it’s a lot easier to dose-reduce zanubrutinib.
SILVA: [It could even lead] to developing resistance. They might respond initially, but…[if] it’s affecting pharmacokinetics, you might not have as long of a response.
AYOOLA: For the primary trial that got ibrutinib approved, what percentage of patients had dose reduction? If they were dose-reducing to [280 mg daily] and the final analysis was for the intention-to-treat [population], if everybody was included and everybody did well, [then dose reductions] didn’t matter.
MARKS: I don’t know in the original trial exactly how many had dose reduction, but we did a real-world study at the University of Pittsburgh Medical Center [in Pennsylvania] in terms of patients discontinuing ibrutinib. Surprisingly, it was almost one-third of patients who came off ibrutinib, even with dose reductions.5 There’s no question that of the 3, ibrutinib is the most poorly tolerated for a whole host of AEs, including the cardiac AEs, the bleeding, and even the minor things such as fatigue, bruising, diarrhea, etc.
DISCUSSION QUESTION
- Other than cardiac AEs, how do other safety concerns affect your choice of BTK inhibitor?
MARKS: How do other safety concerns affect your choice? In my experience, I saw the most AEs with ibrutinib besides the major cardiovascular [issues], hypertension, etc.
REMTULLA: I’ve seen quite a lot of dermatitis associated with ibrutinib compared with the newer BTK inhibitors. I haven’t seen it with acalabrutinib or zanubrutinib. [This is] lifestyle-limiting dermatitis [that is] diffuse.
BARSOUK: I’ve seen asthenia, fatigue, and cytopenias more with ibrutinib.
APOSTOLOVA: Bruising has been a little more pronounced in my experience with ibrutinib.
MARKS: I agree with you. Bruising is a lot greater with ibrutinib than with any others. What about the headache with acalabrutinib? [Approximately 35% of] patients who start acalabrutinib get a headache.2 It’s transient in most patients and relieved with caffeine. But there are patients who have persistent headaches on acalabrutinib, which I haven’t seen with zanubrutinib. One of the other AEs… is secondary malignancies. The primary one is nonmelanoma skin cancers.1,2
AYOOLA: I had a patient who I’ve treated with both acalabrutinib and obinutuzumab. He has been on acalabrutinib for probably 2 to 2.5 years, and he showed up in my clinic with a mass in the liver that turned out to be metastatic neuroendocrine carcinoma. I asked [the drug manufacturer] to give me the list of secondary malignancies that have been associated with acalabrutinib, so I am still taking a look at that. I know you can get solid tumors, melanoma, and nonmelanoma skin cancers, but I am not sure whether neuroendocrine carcinoma has been associated [with BTK inhibitors].
MARKS: Interesting. Obviously, patients with CLL have a much greater incidence of nonmelanoma skin cancers. But at least in [findings from] the acalabrutinib trials, it looks like the incidence is greater than with the other BTK inhibitors.2 The jury’s still out, but it’s an area of concern. We want to have our patients routinely monitored by dermatologists, particularly when they’re on a BTK inhibitor. That’s another safety concern to take into consideration.
DISCUSSION QUESTION
- How do you interpret the efficacy and safety outcomes of the ALPINE (NCT03734016) and ELEVATE-RR (NCT02477696) trials?
MARKS: ALPINE was zanubrutinib vs ibrutinib. ELEVATE-RR was acalabrutinib vs ibrutinib in the patients with high-risk cytogenetics. How do you interpret the efficacy and safety outcomes? At least in the ALPINE trial [findings], zanubrutinib was more efficacious than ibrutinib, whereas in the ELEVATE-RR trial [findings], they look to be equivalent in terms of progression-free survival [PFS]. Both acalabrutinib and zanubrutinib seem to have a lower risk of atrial fibrillation and flutter vs ibrutinib [Tables 1 and 21,2].
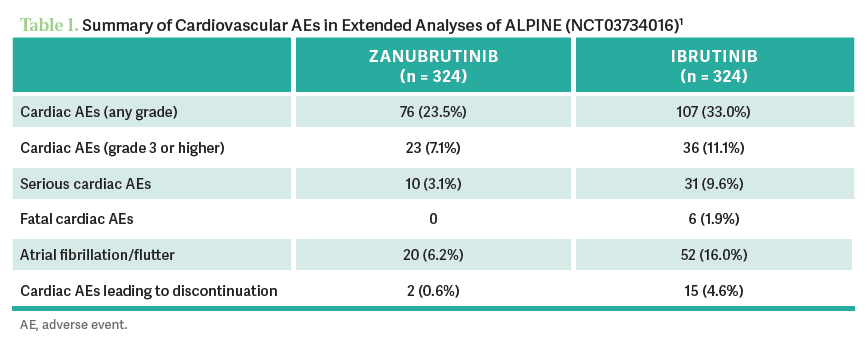
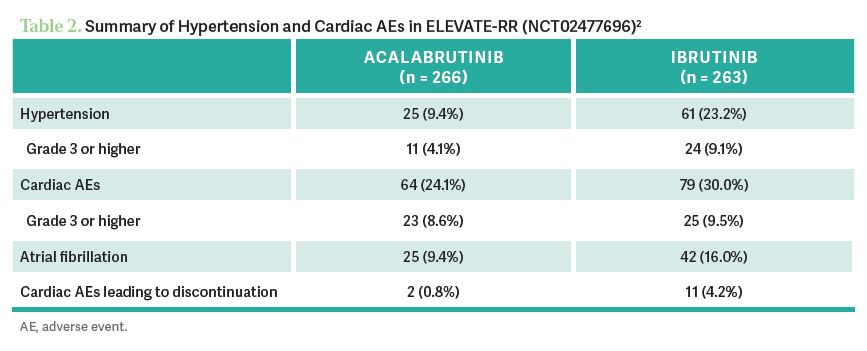
SILVA: The number that I tend to memorize and quote to patients when I’m trying to pull patients from ibrutinib—I still have patients who are taking it and don’t want to stop it—[is] a 16% incidence of atrial fibrillation vs 9% with acalabrutinib and less than 5% with zanubrutinib.1,2 Although I had 1 patient who was fine on ibrutinib for [a long time], and I started him on acalabrutinib, and the next week, he had atrial fibrillation.
REMTULLA: Should we strive to change [regimens for] patients who have been stable on ibrutinib for 2 years to one of the newer drugs?
MARKS: No, it’s not recommended, unless they’re having toxicity or intolerance.
BARSOUK: I had situations like this where patients were on ibrutinib and responding but had intermittent atrial fibrillation. In those patients, I would switch, but in a patient tolerating ibrutinib well, if it’s not broken, I’m not trying to fix it.
MARKS: And if they have atrial fibrillation before they’re diagnosed, what would you do?
BARSOUK: For preexisting atrial fibrillation, I would not offer ibrutinib to begin with. But I barely use it at all, so that’s a moot point. I can’t imagine [to] whom I would offer ibrutinib and not second generation nowadays. I don’t think there are patients like that.
APOSTOLOVA: I had 1 patient where insurance did not approve anything else until they failed [to respond to] ibrutinib.
DISCUSSION QUESTION
- Do you think PFS is a relevant end point in CLL?
BARSOUK: Yes. It’s the closest surrogate to overall survival [OS], and it’s very difficult to demonstrate OS difference. These trials only have several years’ follow-up…so that is impossible, and…you need to have much more mature data to see OS. In the meantime, even for patients [in the] second line, PFS is also related to quality of life. Patients can be in remission while continuing the drug, such as in a chronic disease, and you postpone the progression or need to switch therapy. This is clinically relevant.
REFERENCES:
1. Brown JR, Eichhorst BF, Lamanna N, et al. Extended follow-up of ALPINE randomized phase 3 study confirms sustained superior progression-free survival of zanubrutinib versus ibrutinib for treatment of relapsed/refractory chronic lymphocytic leukemia and small lymphocytic lymphoma (R/R CLL/SLL). Blood. 2023;142(suppl 1):202. doi:10.1182/blood-2023-174289
2. Byrd JC, Hillmen P, Ghia P, et al. Acalabrutinib versus ibrutinib in previously treated chronic lymphocytic leukemia: results of the first randomized phase III trial. J Clin Oncol. 2021;39(31):3441-3452. doi:10.1200/JCO.21.01210
3. Brukinsa. Prescribing information. BeiGene Ltd; 2024. Accessed March 25, 2024. https://tinyurl.com/v4upwbbf
4. Calquence. Prescribing information. AstraZeneca; 2022. Accessed March 25, 2024. https://tinyurl.com/2vs945cy
5. Hou JZ, Ryan K, Du S, et al. Real-world ibrutinib dose reductions, holds and discontinuations in chronic lymphocytic leukemia. Future Oncol. 2021;17(35):4959-4969. doi:10.2217/fon-2021-0964

Leon-Ferre Explores Targeting of PIK3CA Alterations in ER+ Breast Cancer
July 24th 2024During a live Community Case Forum event in partnership with the Minnesota Society of Clinical Oncology, Roberto A. Leon-Ferre, MD, discussed drugs targeting PIK3CA alterations in patients with ER+ metastatic breast cancer.
Read More
George Explores Impact of Risk Status With Cabozantinib/Nivolumab in Advanced RCC
July 19th 2024During a Case-Based Roundtable® event, Daniel George, MD, discussed the results of the CheckMate 9ER trial across favorable, intermediate, and poor risk groups in patients with advanced renal cell carcinoma.
Read More
Rossetti Reviews Myelofibrosis Risk Stratification and Outcome Data for Pacritinib
July 17th 2024During a Case-Based Roundtable® event, James M. Rossetti, DO, discussed the role of risk scoring and stratification tools and treatment for a patient with declining hemoglobin and platelet counts due to primary myelofibrosis.
Read More