Case 1: GvHD Background
Episodes in this series

Corey Cutler, MD, MPH, FRCPC: Thank you all for joining us today for this Targeted Oncology™ Virtual Tumor Board®, which is focused on graft-vs-host disease [GVHD]. In today’s presentation, my colleagues and I are going to review 3 clinical cases. We will discuss our individual approaches to the treatment of each patient, and we will review some key clinical data that helped impact our decisions.
I am Dr Corey Cutler, from the Dana-Farber Cancer Institute and Harvard Medical School in Boston, Massachusetts. I am joined by Dr Dan Couriel from the University of Utah Huntsman Cancer Institute in Salt Lake City, Utah, and Dr Usama Gergis from the Sidney Kimmel Cancer Center in Philadelphia, Pennsylvania.
We will start with a little background on graft-vs-host disease.
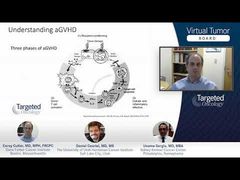
As we all know, GVHD is 1 of the main causes of nonrelapse mortality following allogeneic stem cell transplantation. We have 2 main clinical syndromes that we deal with. Acute graft-vs-host disease is a syndrome that occurs relatively early after transplant, mainly affecting 3 organs and 3 organs only: the skin, the gastrointestinal tract, and the liver. It is caused predominantly by a T-cell–mediated reaction.
Chronic graft-vs-host disease, on the other hand, is a very heterogeneous syndrome that occurs months to even years following transplantation. It resembles a number of immunologic or autoimmune diseases and is a unique syndrome in each patient it’s affecting. It really has long-term implications on the quality of life for the patients affected.
The risk factors for acute and chronic GVHD are quite similar, and acute GVHD was once thought to be the main risk factor for the occurrence of chronic graft-vs-host disease. About 25% to 50% of patients who get transplants from well-matched donors will have acute or chronic graft-vs-host disease requiring systemic therapy, and a number of patients who require systemic therapy unfortunately have inadequate responses to corticosteroids. Both are associated with very poor prognoses, and there are requirements for a number of other immunotherapeutic targeted approaches.
When we talk about graft-vs-host disease, almost all our patients require some form of prevention for GVHD. Shown on this slide are a number of molecular pathways and targets that we use to try to prevent graft-vs-host disease. It turns out that most of these pathways are also active when we are talking about treating acute graft-vs-host disease. The standard of care in North America is generally the combination approach for the prevention of acute graft-vs-host disease. In North America, most patients will receive a combination of a calcineurin inhibitor, either tacrolimus or, less commonly, cyclosporine in combination with an antiproliferative agent, most commonly represented by methotrexate but sometimes represented by mycophenolate mofetil. There are a number of other agents that are out there. For some of them, their pathways are shown here.
This slide really shows 1 of the seminal phases of acute GVHD pathways. This was devised by Drs Joseph Antin and James Ferrara over 3 decades ago, and it speaks to T-cell activation in the context of exogenous or even internal stimuli for upregulation of the immune response. It involves upregulation of T-cell activity and cytokines that upregulate this entire pathway, finally leading to the elaboration of polysaccharide and other types of inflammatory markers and immune attack on target tissues. Despite being over 30 years old, this is still a model that we actively use today.
In terms of risk factors, the most important risk factors are HLA [human leukocyte antigen] related. But as stem cell–transplant physicians, some other things we can manipulate are choosing donors who are younger and trying to minimize older donors. We try to minimize sex mismatch when we choose our stem cell donors. We can choose the preparative regimen intensity, understanding that regimens with higher intensity are associated with more graft-vs-host disease and understanding that the regimens that use high-dose radiation are also associated with higher rates of graft-vs-host disease.
This slide demonstrates the agents we commonly use for prevention. As I mentioned before, the calcineurin inhibitors and methotrexate are used most commonly at our institution and at several others. The mTOR inhibitor sirolimus is commonly used. There is increasing use of the agent cyclophosphamide to prevent graft-vs-host disease. This has been pioneered by physicians at Johns Hopkins in Baltimore and has predominantly been used in haploidentical transplantation, but more recently it has started to be used in unrelated donor transplantation. Then, of course, at the end of this slide, clinical trial agents speak to the fact that the real way we are going to improve outcomes in transplantation is really with the use of large, well-designed, and randomized clinical trials to test novel agents and novel strategies to prevent graft-vs-host disease.
A number of strategies are being used. In addition to the pharmacological agents, we are attempting to modulate stem cell grafts, either with the depletion of all T cells or selective depletion of T cells. We are also doing graft modulation before the cells are infused. We are exploring a whole other category of drugs that modulate T-cell trafficking, preventing the T cells from getting to the target tissues. We are using T cell costimulation antagonists, drugs that prevent the upregulation of T-cell responses. Several other classes of agents are being used, both in the treatment of and for prophylaxis, such as the JAK inhibitors, which we’ll speak about a little later over the course of this tumor board.
Transcript edited for clarity.