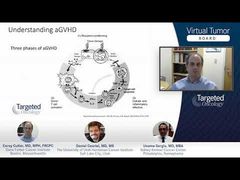
Case 2: Treating Steroid-Refractory Acute GVHD
Episodes in this series

Corey Cutler, MD, MPH, FRCPC: I'm going to ask my colleagues, Dan and Usama, what your initial reactions are and how the publication of REACH2 has changed your practice for steroid-refractory acute graft-versus-host disease [GVHD]? Dan, do you want to lead us?
Daniel Couriel, MD, MS: REACH2 confirmed what a lot of us were expecting to see because all the results that we were seeing preliminarily look pretty promising. I started, to be completely honest, starting ruxolitinib as second-line therapy for steroid-refractory acute GVHD a little before we had this confirmation. It did change my practice because up until then, my go-to choice, particularly for skin and liver, was extracorporeal photopheresis. That’s the technology and the treatment that I was more familiar with. Now, with the advent of ruxolitinib and the approval, I feel that I have a second choice that is just as valid and probably more validated at this point. Needless to say, it helps a lot from an insurance perspective, too.
Corey Cutler, MD, MPH, FRCPC: Usama, your thoughts on this compound and how has it changed your practice?
Usama Gergis, MD, MBA: I agree with Dan and you, Corey. We have to remember that the approval of ruxolitinib almost a year ago for acute GVHD, steroid-refractory acute GVHD, was based on efficacy results in 41 patients, which highlights the unmet need in that arena with all the variables in recipient conditioning and patients without variable disease. It’s impossible to tease out response and efficacy in 41 patients. When this publication came in recently, I think a month or a month and a half ago in the New England Journal of Medicine, most of us were part of this trial, so we were in the know. It’s good to finally have a phase 3 trial.
The other point is even before the approval for ruxolitinib and the publication of the data on the 41 patients, there were 2 retrospective, large reports. Each one reported on almost 100 patients. Again, just like Dan said, we were, way before the approval, giving ruxolitinib in that setting, but you really have to go through hoops sometimes with logistics and insurance. It’s good to have solid data.
Corey Cutler, MD, MPH, FRCPC: What were you using before ruxolitinib? What was your go-to second-line agent? Was it the same in all patients, or did it depend on the clinical scenario, like Dan mentioned that he used extracorporeal photopheresis predominantly in cutaneous and hepatic disease?
Usama Gergis, MD, MBA: One, we are all products of our experiences or posttraumatic stress syndromes that we have from our patients who sometimes do not do well with certain things. My early experience was really marked by losing patients from lower gastrointestinal [GI] acute GVHD, so my first choice for skin, GI, and liver were, if no clinical trials were available and we’d done mesenchymal stem cells—we’d done many clinical trials—was for ECP [extracorporeal photopheresis] with or without something else. I’ve always been a believer in ECP because it’s not pharmacologic and, as you said, does not affect blood counts. It is, of course, logistically difficult for patients to have a catheter and come twice a week sometimes, but the short answer is that clinical trials are number one: no clinical trials, ECP with or without something else.
I’m also a fan of the local steroids for the upper beclomethasone and budesonide to treat the GI. I use that liberally. That is basically my practice.
Corey Cutler, MD, MPH, FRCPC: And it is interesting because we use very little ECP here in our center for steroid-resistant acute GVHD, and the difference in our practice is that it is not based on data. It is simply based on this is what we do here. We do have access to ECP, but it simply was not part of our culture, if you will, but it was freely available, and we do use it sometimes, I will admit, particularly in patients who we are more concerned about regarding infection. Because, as you mentioned, it is not immunosuppressive.
Again, I think the 3 of us all agree that clinical trials are still the mainstay. It is possible now that ruxolitinib becomes the control arm for these clinical trials as new agents are being developed, and I think we will all agree that having an agent with demonstrated efficacy as the control will make us much more comfortable testing agents, knowing that the control arm is going to be getting active therapy, and we now have a higher hurdle to get across to get new agents approved.
Daniel Couriel, MD, MS: Right, and I wanted to add my shared practice with you, Usama, of oral beclomethasone. Before REACH2, oral beclomethasone was probably the only agent with a randomized study that you could base your practice on, so I do use it in situations where I can use it.
Transcript edited for clarity.