Case 3: Treating Chronic Graft-Versus-Host Disease
Episodes in this series

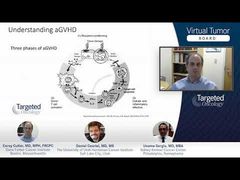
Bart L. Scott, MD: This is a very interesting and difficult case where a patient has developed sclerodermatous changes of the skin, muscle and joint pain, as well as dry eyes and vaginal dryness. All of these symptoms would be consistent with chronic graft-versus-host disease [GvHD].
The treatment options are many. One would be oral methotrexate. That has been helpful in patients who have joint pain, for instance, in particular. Another option would be imatinib. That can be helpful in patients who have sclerodermatous changes. Ibrutinib is FDA-approved for treatment of chronic GvHD. Ruxolitinib has also been shown to be effective in clinical trials for treating patients with chronic graft-versus-host disease.
I think there are multiple treatment options for this patient, and it can be difficult to know what would be best in a given individual. We need further studies with randomized trials to be able to answer this question definitively.
Ibrutinib and ruxolitinib are choices for treating this patient. I can’t necessarily say which of those drugs would be best. I have more experience with ruxolitinib. I think the adverse effect profile of ruxolitinib might be a little better than what you experience with ibrutinib, but I think both of those would be potential choices in the treatment of this patient. I don’t think we can say for sure which would be the best choice.
I would generally start this patient on 1 mg/kg of steroid therapy. Does a more aggressive starting dose improve outcomes? I think that’s a question that we don’t know the answer to for certain yet, and we need further trials to be able to answer that question definitively.
Certainly there are adverse effects from high-dose steroids. Patients who are treated with chronic GvHD with steroid therapy tend to have a longer duration of treatment. I generally look at a variety of different factors in determining which dose of steroids I would start on a patient. For example, do they have thrombocytopenia, which is a negative risk factor? Do they have a significant eosinophilia, which is a negative risk factor? What’s the total body surface area that’s involved with sclerodermatous changes?
So if they appear to have more organ involvement, more severe form of chronic GvHD, then I would generally give them a higher dose of steroid therapy. With chronic GvHD, we tend to do a more prolonged taper.
This patient is developing sclerodermatous changes, and the patient is also developing dry eyes and vaginal dryness. There are topical ointments that should be applied to both the vagina and the eyes to help with the dryness. In regard to the sclerodermatous changes, physical mobility is very important. Involving physical therapy and teaching the patient exercises so that they can continue movement as much as they are able to is an important component of management of this patient as well as also sticking to a daily exercise routine for the patient.
Sun exposure can worsen GvHD symptoms and also increase the risk of skin cancer, for which patients who receive an allogeneic transplant are already at increased risk. The patient can wear protective sunscreen when outside. This would also be an important component of their management.
Transcript edited for clarity.