Case 3: Treating Moderate Chronic Graft-Versus-Host Disease
Episodes in this series

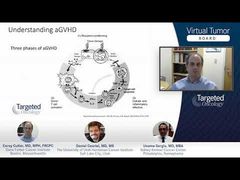
Daniel Couriel, MD, MS: I use the same system that we've used in the presentation, which is the NIH [National Institutes of Health] consensus grading system, updated in 2014. This was the first structured effort to better define what constituted chronic GVHD [graft-versus-host disease] from a clinical perspective and also tried to make sense of stratification of severity. This is a moderately severe case of chronic GVHD. It a complex scoring system, just like the disease. The scoring is based on 2 things: one is the severity of involvement of the organs in question. The second is the number of organs involved. That is how we get to an overall grade that defines whether the patient is in the mild, moderate, or severe category.
In general, the way we approach these different categories, the mild categories are handled without systemic therapy, if possible, which is what happened in the case of this woman. Then, once we move into the moderately severe or severe levels, we offer systemic therapy. Ideally, that systemic therapy would be within a clinical trial, and in the absence of a clinical trial, is prednisone at a dose of 1 mg/kg per day.
Corey Cutler, MD, MPH, FRCPC: Do you do prednisone at a mg/kg, and do you give a calcineurin inhibitor with the prednisone when you start systemic therapy?
Daniel Couriel, MD, MS: That's an excellent question. I do use 1 mg/kg/day, yes. I do think, and this is largely empirical, that GVHD is a very time-dependent disease. As time goes by, I think that you lose ground. I try to be aggressive up front, and I do use the mg/kg. When I decide to treat, I treat, and as far as the calcineurin inhibitor, I do use it as well because although it has not been proven to increase the efficacy of the steroids, it has shown steroid-sparing capacity and fewer long-term steroid-related complications, which become a huge problem over time. It blends into the syndrome of chronic GVHD, so I do use them as well.
Corey Cutler, MD, MPH, FRCPC: Usama, what about you?
Usama Gergis, MD, MBA: I do more or less the same, the 1 mg/kg but with a fast taper. Again, I am a fan of ECP [extracorporeal photopheresis] for chronic GVHD, so I jump into ECP earlier. Depending on the timing, if my patient does not respond fully, and obviously steroids are very toxic, I can add other agents. If it is earlier on, let's say the first 6 months or so, most of our patients will be already on a calcineurin inhibitor, so it hasn’t even been stopped. After a year and a half, it will be a case-by-case basis.
Corey Cutler, MD, MPH, FRCPC: What are your thoughts on the CTN [Clinical Trials Network] study that looked at sirolimus with a tacrolimus withdrawal approach to foster regulatory T cells? Is that something either of you have adopted into your practice? I am talking about CTN 0801.
Usama Gergis, MD, MBA: I have not. I use sirolimus sparingly. Culturally, in my practice, whether in New York or here, I have not adopted this as an algorithm.
Daniel Couriel, MD, MS: I haven't adopted it either, yet. Because it is a big change in practice, and I'm not saying that the idea behind this CTN study is not great, I think that the size or the magnitude of the change in practice is directly proportional to how much data you need to see on that particular topic. I think that I need to see more to change my practice to using sirolimus that way.
Corey Cutler, MD, MPH, FRCPC: Your patient now is 2 months on corticosteroids at a healthy dose of 1 mg/kg, and the scleroderma is not better. In fact, perhaps it is even worse. What do you reach for next?
Daniel Couriel, MD, MS: Two months is probably a little more than I would wait, but let's go with the 2 months. At this point, I would definitely go to an additional agent. As we all know, we look at 2 things in these agents. One is efficacy, and the second one is steroid-sparing capacity. The first thing I look at is if there is a clinical trial because our standard therapies are, of course, less than optimal. If I don't have a clinical trial, my go-to treatment would be ECP, which does have a good track record in the treatment of sclerodermatous forms of chronic GVHD.
Corey Cutler, MD, MPH, FRCPC: Usama, what about you?
Usama Gergis, MD, MBA: I would have gone to ECP earlier than the 2 months. One mg/kg for 2 months is a very long time. It’s a huge cumulative dose for, I forgot how old this man is. Well, luckily, he's younger. He's 35. I would have gone to ECP much earlier. Ibrutinib is a drug that we can use. Obviously, clinical trials are the first choice. It's becoming a cliché now after we’ve said that too many times. It should be where we go first.
Transcript edited for clarity.