Case 1: Transformation of Myelofibrosis to AML
Episodes in this series

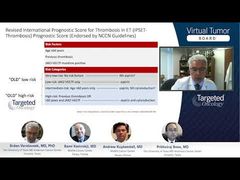
Srdan Verstovsek, MD, PhD: It seems to me that we are moving to putting a lot of weight for these additional mutational abnormalities in terms of prognosis. Rami, you have shown a couple of new prognostic scoring systems that incorporate molecular factors and even dissect the patients with mild fibrosis in different groups from those that are secondary to ET [essential thrombocythemia] or PV [polycythemia vera] to mild fibrosis or primary. How do we choose among all these? You showed only a couple and there are many more. Why not also talk about the risk of transformation to acute myeloid leukemia [AML] as a valid point for prognostication? How do we go with choosing the best and expanding to utilizing them perhaps to see who is going to transform to AML?
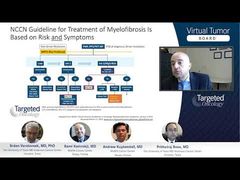
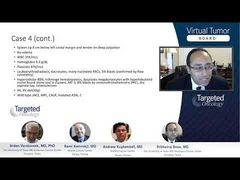
Rami Komrokji, MD: I think that’s a good point. Obviously, there is a lot of overlap between those risk models, and obviously, there are common variables that we can use in those models. Some of them are depending on a clinical phenotype, some of them are depending more on molecular phenotype. To keep in mind also that part of the clinical phenotype, sometimes it’s more flexible than molecular phenotype as well. Having said that, I think in practice, we usually start with something like the DIPSS [Dynamic International Prognostic Scoring System] or DIPSS-Plus because it is more comprehensive, and we do complement it with 1 of the genetically based models like the MIPSS70. Actually, Dr Kuykendall published some of our work looking at when we had a discrepancy between 2 stages difference, between somebody that in a clinical-based model, had, let’s say, a low risk, while a genetically inspired model was intermediate-2. It seems that the genetically inspired model did find the prognostic value. So, especially in the younger patients, as after doing the clinical model, I tend to use the MIPSS70-Plus, for example, in deciding particularly if those patients have enough risk features of the disease to consider allogeneic stem cell transplant.
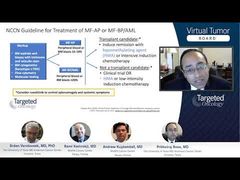
Your point is well taken. I think we have to start looking more also about the risk of AML transformation. There are obviously certain predictors that are clinical, as well as molecular, that can help us to predict the risk of transformation in AML. Maybe as Andrew was alluding, that could be a population down the road that we would be considering for an allogeneic stem cell transplant earlier or intervention. For example, the group that has IDH-1/IDH-2 mutations is known to be at higher risk for transformation, and maybe those are the patients who we should be considering to receive some treatments earlier.
Transcript edited for clarity.