Case 4: MPN Transition From Chronic- to Blast-Phase MPN
Episodes in this series

Prithviraj Bose, MD: With therapy, unfortunately, the story is quite dismal. This shows you work from Ruben Mesa from 15 years ago, showing that the survival is really very abysmal with conventional AML [acute myeloid leukemia]–type chemotherapy. In fact, the only ones that can have any long-term chance of survival are those who have a remission and then an allogeneic stem-cell transplant, not shown on this slide. But this just shows you that in general, chemotherapy is very poorly effective.
For azacitidine, the French looked at this about 10 years ago. This was a group of about 50 patients that either had AML or MDS [myelodisplastic syndrome] arising from MPN [myeloproliferative neoplasm]. MPN can also transform to MDS, about half and half. You see here that the azacitidine had a decent response rate of about 52%. Obviously, this is a highly established drug in both AML and MDS, so here too you have a reasonable response rate, 24% CR [complete response], 11% PR [partial response], and some MLFS [morphologic leukemia-free state]–type responses.
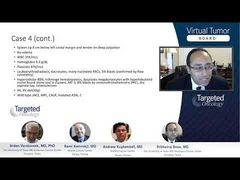
Just to remind you about this, there is something we call accelerated phase. It’s not particularly well established in the literature, but the only thing that seems to be clear to define it is this blast percentage, whether in the blood or in the marrow, of 10% to 19%. It seems to define this intermediate phase, which has an intermediate prognosis between chronic and blast phase but clearly is heading in the wrong direction. Again, blasts pretty much define accelerated phase in the 10%-to-19% range.
This shows you that most MPN patients who go from chronic phase to blast phase actually transit through the accelerated phase, with very few going straight from the chronic phase to the blast phase. This is work from our institution from a number of years ago.
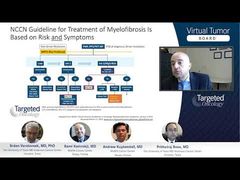
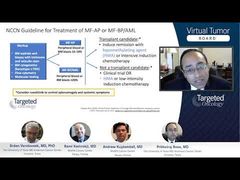
Regarding the NCCN [National Comprehensive Cancer Center] Guidelines, we saw that chemotherapy doesn’t work very well at all. Transplant is the goal if you can get there, so you need to induce remission.I don’t think it’s very important how you achieve remission. But whether it’s an HMA [hypomethylating agent] or chemotherapy, if you can get them to remission and get them to allogenic stem cell transplant, that is really your only realistic hope of long-term survival. For those for whom that’s really not an option, frankly, chemotherapy doesn’t seem to have much of a role because you’re going to invite toxicity without much benefit. In those patients, a number of groups, including us, like to use ruxolitinib with the HMAs in part to control the spleen symptoms, etc. For those patients, it’s a very deliverable outpatient, relatively easy regimen, and that’s probably the way to go for those who are not going to a transplant. Of course, needless to say, a clinical trial is probably your best bet.
This is what I was touching on a little earlier. Our group at The University of Texas MD Anderson Cancer Center and our friends in New York have looked at ruxolitinib and decitabine in somewhat different dosing strategies. But unfortunately we came up with the same disappointing survival outcome of around 7 months median survival. This is a drug combination that is easier to deliver and perhaps gives patients some quality of life above what chemotherapy might achieve.
Transcript edited for clarity.