Case 3: Risk Assessment of Essential Thrombocythemia
Episodes in this series

Srdan Verstovsek, MD, PhD: We are all talking about the risk assessment for thrombosis, and that can change over time because it’s not only that we age and you get to 60 and then we always joke about giving a patient a prescription for a cytoreductive therapy when they have a birthday. But there are other factors that do evolve, other comorbidities. How do we go about proper assessment of the patients during their life? Rami, how would we go about it? We said no bone marrow biopsies. What other factors are we looking for to say, “You changed, you need to do something different?” It’s not only platelets, right?
Rami Komrakji, MD: Definitely, yes. Again, we would be thinking the same thing in 2 terms: a risk of thrombotic events and a risk of disease progression. Obviously, if somebody had a thrombotic event, then that will change the risk. I think it’s a good idea to also keep an eye on the cardiac risk factors for those patients. If there is anything changing there, then the risk of arterial events is probably going to increase. There is also a change in some of the blood counts. For example, I think leukocytosis could sometimes be predictive or correlates with thrombotic events more than a platelet count, per se. So, I would say from the risk of thrombotic events, those are the things I look at—if the patient obviously has had a thrombotic event, if they are having any other cardiac risk factors, and if there is change in other blood counts or inflammatory conditions that could set a thrombotic event.
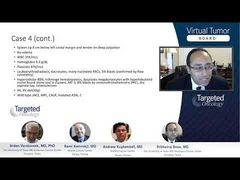
In terms of the disease outcome, obviously if we start seeing cytopenias, anemia, circulating blasts, which are not common in ET[essential thrombocythemia]—but the anemia, high LDH [lactate dehydrogenase]—those are probably flags to start thinking: Is this disease progressing to post-ET MF [myelofibrosis]? Should we reassess? Disease risk is changing at that point.
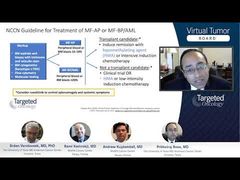
Srdan Verstovsek, MD, PhD: Excellent. Then, in many of these cases, you would then say, either because the white cells are high or the thrombotic event happened or the spleen is increasing, we may need to start the cytoreductive therapy, or the patient is just older and it’s time to start therapy. Hydroxyurea is the first-line therapy, but interferon still has a role. Prithviraj, what is your take on interferon here? Unlike PV [polycythemia vera], in ET guidelines, it says hydroxyurea first, interferon later on.
Prithviraj Bose, MD: Right. As we were discussing earlier, I tend to reserve interferon for the younger patients who obviously have a much longer duration of therapy that lies ahead of them. But I put a lot of faith in the MPD-RC trial that actually found no difference between hydroxyurea and interferon at 2 years in the front-line setting in PV or ET. So, in general, I stick with hydroxyurea, but I do use interferon in my younger patients where you have more of a concern for the long-term toxicities of hydroxyurea.
Srdan Verstovsek, MD, PhD: Andrew, how about anagrelide? There are studies of anagrelide versus Hydrea. Some show that Hydrea might be better for some particular characteristics that happen in patients with ET; others say it’s about the same.
Andrew Kuykendall, MD: I think we haven’t used anagrelide that much, but it is effective in managing platelet counts. Early on, there were some studies—1 major study showed that hydroxyurea was superior to anagrelide, especially for preventing arterial events. But there was a concern that potentially using different diagnostic criteria, that was enrolling a more high-risk patient population, and then more recent studies suggested noninferiority between the 2. But I would say overall, hydroxyurea has more potential benefits of its use and it’s largely tolerated better than anagrelide, but certainly anagrelide can be considered in some patients who are either not able to tolerate Hydrea and interferon, and it can reduce the platelet counts.
Srdan Verstovsek, MD, PhD: Once we start the cytoreductive therapy, I think we all agree that we are not only looking at the control of the platelets, but white cells if they are elevated, the symptoms if they are present, and the spleen if it is present. The goal of therapy has broadened to include multiple factors as in polycythemia vera. Once you perhaps control the platelets, but not the others, Rami, is there a time then to change, or you are satisfied with just controlling the platelets? How do you manage the need for a second therapy?
Rami Komrakji, MD: That’s a very challenging question because I really don’t think there is a good correlation between the platelet count, and we don’t even know the goal that we should get the counts to. I don’t think there is good correlation between the baseline or getting the counts controlled, but we all try to get the platelet count as normal as possible. I do pay attention to leukocytosis, I think that’s an important element. Also, as we mentioned, we are watching to see if there is any change in terms of the risk factors, the risk of thrombosis for those patients. But definitely, platelet count alone is not what I look at because I really don’t know what is the target or the goal in those patients. So, leukocytosis is definitely relevant to look at and obviously patient tolerability as well.
Transcript edited for clarity.