Case 4: Assessing Risk for Transformation to AML
Episodes in this series

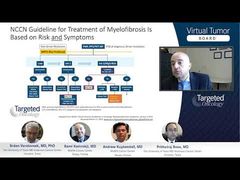
Srdan Verstovsek, MD, PhD: Let’s start the discussion with what are the risk factors for the transformation. Many of these risk factors overlap to a great extent with risk factors that are accounted for in prognostication of overall survival of the patients, and the prognostications for overall survival primarily is used to define the patients that could be going to a transplant as if they have a life expectancy of less than 5 years.
It seems to me that there is a good case to prognosticate for transformation to myeloid leukemia, but it doesn’t really appear that we can do much about it. Andrew, what do you think about that? Is there a real need for everyday practice to prognosticate for not only survival but also acute myeloid leukemia risk?
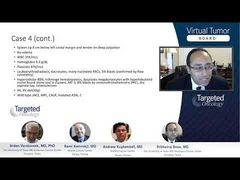
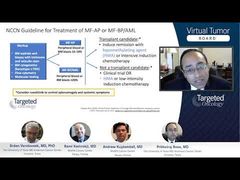
Andrew Kuykendall, MD: Yeah, I think so. Certainly, if we were able to identify patients who, in the chronic phase, were at high risk of transformation to acute leukemia, those would be the patients we would rapidly take to transplant to see if we could prevent that. As Prithviraj discussed, once the transformation occurs, it’s really challenging to get those patients back to a state of their disease that’s then transplantable with any kind of success rate. I think it’s important to take that into account, and certainly our prognostic models, in myelofibrosis specifically, look at overall survival. But certainly some of those risk factors that we include in prognostic models exert their impact on overall survival by increasing the risk of transformation, and we touched on some of those, like thrombocytopenia, cytogenetic abnormalities, and certain mutations as well. So I think it is important to do that.
Srdan Verstovsek, MD, PhD: Prithviraj, in ET [essential thrombocythemia] and PV [polycythemia vera], you mentioned at the beginning that the risk of acute myeloid leukemia [AML] is very small, but some patients obviously will have it. While we focus so much on thrombotic risk assessment, we don’t really talk much about the prognostication in terms of transformation to myelofibrosis or acute myeloid leukemia in ET and PV. Should we start doing that?
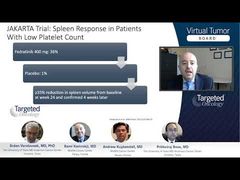
Prithviraj Bose, MD: You know, Srdan, I think the problem with it is that in the absence of a therapy that’s going to retard or delay or prevent that from happening, it perhaps has less practical relevance. Certainly patients will progress either through an MF phase or directly to AML. But when you are starting out treating them for PV or ET, all you can really do is focus on thrombotic risk—symptoms, spleen, things like that. That’s perhaps the reason that we have tended not to do that, and fortunately, it is still a very small risk for PV and ET, which obviously have long life expectancies otherwise. That’s really the driver of that. If we had a drug or a strategy that could reverse this process, certainly it would be more relevant.
Srdan Verstovsek, MD, PhD: Apart from possible implementation of prognostic factors in myelofibrosis, perhaps more than in ET and PV, for transformation to acute myeloid leukemia, there is not much else we can do. We know that the JAK inhibitors do not prevent progression from acute myeloid leukemia, but they don’t enhance the risk either. They’re just controlling the proliferation and inflammation, but they don’t change the possibility of a change.
Transcript edited for clarity.