Case 4: A 68-Year-Old Man With Primary Myelofibrosis
Episodes in this series

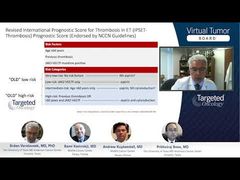
Prithviraj Bose, MD: The fourth case talks about post-MP [myeloproliferative disease] and AML [acute monocytic leukemia], or the blast transformation from primary myelofibrosis [MF]. We’ll start with the case here, a 68-year-old man who was diagnosed with primary MF about 3 years ago but is otherwise healthy. He has a fully matched donor, a sibling donor. He has mild night sweats, weight loss over the last 3 months of 10 pounds, some early satiety, some spleen-related symptoms in the left-upper quadrant, a lot of bone pain. So there are quite a few symptoms and splenomegaly as you see here, some aquagenic pruritus, fatigue, and some wasting.
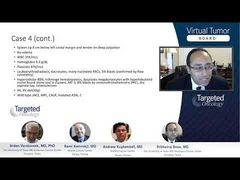
The spleen is enlarged on exam; it’s 8 cm below the left costal margin. The white blood cell count is elevated at 35, hemoglobin is less than 10 g/dL, it’s 9.2 g/dL, platelets are quite low, less than 50 per mm3. Also leukoerythroblastosis, the teardrop cells that are fairly classic for primary myelofibrosis, with 5% circulating blasts in the blood. The bone marrow shows 80% cellularity, trilineage hematopoiesis, dysplastic megs, and a grade 3 fibrosis on a scale of 0 to 3. Eight percent blasts by immunohistochemistry and osteosclerosis. The cytogenetics show the relatively benign del20q, which is actually the most common chromosomal abnormality in primary myelofibrosis, and not a bad one to have. But then you also have the ASXL1 mutation, which is an adverse prognostic one that we’ve been mentioning, and also this case is triple negative.
The patient begins RUX [ruxolitinib]. After 1 month, as you commonly expect, the symptoms and spleen are better. The drug does work very quickly, particularly with symptoms, and this patient is better in a month. However, 8 weeks later, the anemia has worsened. Hemoglobin was 9.2 g/dL; now it’s 8.6 g/dL. The splenomegaly has worsened, and, unfortunately, the blasts have climbed from 5% to 48% in the circulating blood.
Transcript edited for clarity.