Case 3: Low- to Intermediate- Risk Essential Thrombocythemia
Episodes in this series

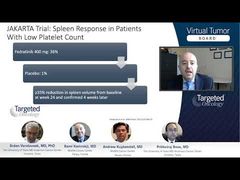
Srdan Verstovsek, MD, PhD: This is 1 of the studies that I like to highlight when we talk about the therapy. We talk about cytoreductive therapy as something that is standard practice for high-risk patients, but many of us in the community setting are nervous when we see, let’s say, a 45-year-old gentleman with high platelets of 1 million or 1.2 million, and say, “Wow, that is not a good number, you are at a high risk of a blood clot and we should treat that patient with cytoreductive therapy.” This is a study published not long ago in 1 of the leading journals, randomizing patients aged 40 to 59 years who had ET [essential thrombocythemia], with high platelets up to 1.5 million, without the high-risk features. In this setting, randomization that was between hydroxyurea or nothing—just of duration—proved the point that normalization of the platelets, which was accomplished with hydroxyurea, did not provide any substantial benefit. In other words, high platelets, up to 1.5 million, in patients with an otherwise low risk, younger than 60 years, no history of thrombosis, does not really provide the benefit.
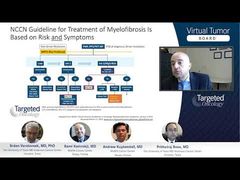
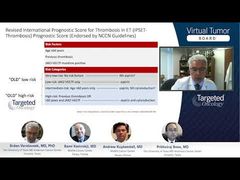
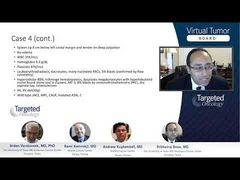
One more point, which is perhaps important for every practice, is the issue of progression from ET to myelofibrosis. Now, we all say that there should be no fibrosis in bone marrow and diagnosis for patients with ET, and that’s correct. They may have some grade of fibrosis later on in their life, if you repeat the bone marrow biopsy after 10 or 20 years. But some presence of fibrosis on its own, it’s not good enough to call the patients transformed. As you see on this slide, there needs to be in addition to change to high-grade fibrosis, anemia or leukoerythroblastic or a big spleen or systemic symptoms or high LDH [lactate dehydrogenase]—all the known factors that are part of the diagnostic criteria for myelofibrosis.
But this is 1 of the practical points, that later on in the life of patients with ET, there might be some fibers in the bone marrow, and maybe these patients are at the risk of transformation to myelofibrosis, but they are not yet transformed because you need to fulfill those factors here to really call the patient transformed. But that’s the other end point of the life of patients with ET, who worry about progression to myelofibrosis: that may happen in a small proportion of the patients, perhaps 5% to 10% of patients do that.
Transcript edited for clarity.