Case 3: A 39-Year-Old Female With Essential Thrombocythemia
Episodes in this series

Srdan Verstovsek, MD, PhD: Case number 3 is a case of essential thrombocythemia [ET]. This is a 39-year-old woman with elevated platelets in the range of 475 × 109/L that were detected on an annual physical exam. The patient was, at the same time, found to have a hemoglobin level of 12.7/dL
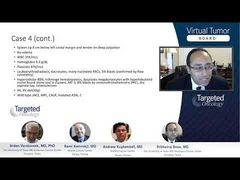
and white blood cell count of 9.9 × 104/L, which are within the normal range. The bone marrow biopsy was then done, revealing proliferation of megakaryocytes with elevated numbers of enlarged, mature megakaryocytes in the bone marrow, without any evidence of reticulin fibrosis. The molecular testing that can be done not only on bone marrow, but also in blood, did not reveal a BCR-ABL fusion, excluding chronic myeloid leukemia, and there was no JAK2 mutation either, the most common one found in the BCR-ABL negative MPNs [myeloproliferative neoplasms]. This patient actually had a type 1 calreticulin mutation detected.
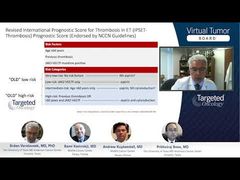
If you look at the diagnostic process for essential thrombocythemia, which is outlined here, we start with the collection of the criteria that would be major criteria, and that would include the bone marrow biopsy. The bone marrow biopsy in patients with high platelets serves the purpose of documenting the disease, looking at the size, shape, and colors of megakaryocytes as we noted before. It also makes sure that we are not facing another disease that many times, patients present similarly with high platelets, which is the early or prefibrotic myelofibrosis. In that case, there would also not be much fibrosis, but there will be some other findings that would be perhaps dependent on the eye of the hematopathologist, to dissect between the 2 types of the diseases in the bone marrow, looking basically at the megakaryocytes themselves.
In each disease and in ET particularly, we would have about 60% of the patients with the JAK2 mutation, about 20 or 25 with calreticulin mutation like this patient, and a smaller percentage of patients with MPL mutations. This is to say that there are patients who have no molecular marker at all in our testing.
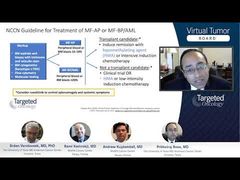
For ET, all 4 major criteria or the first 3 major criteria and 1 of the minor criteria need to be fulfilled, and when we come to dissect the case between the ET or differentiate between ET and prefibrotic myelofibrosis, the key is to see whether there are any of the minor criteria that would help us take away the significance of differentiation from the bone marrow alone, by looking at the blood cell count, LDH [lactate dehydrogenase], and splenomegaly. If these abnormalities are present, then it will make it easier for us to diagnose patients with prefibrotic myelofibrosis.
Transcript edited for clarity.