Case 2: A 67-Year-Old Male With Polycythemia Vera
Episodes in this series

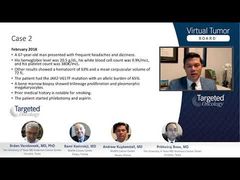
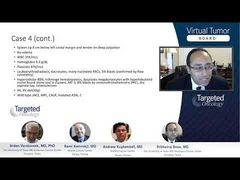
Andrew Kuykendall, MD: For case 2, we’re going to present a case of uncontrolled polycythemia vera. We have a 67-year-old male, who in February 2018 presents with frequent headache and dizziness. His hemoglobin level is very high, 20.5 grams g/dL, and white blood cell count and platelets are kind of high-normal— just a little bit elevated at 9.9cells per cubic millimeter of blood and 380 per microliter. Other results showed a hematocrit level of 63% and some microcytosis, suggestive of possible iron deficiency. The patient has a JAK V617F mutation and allele burden of 65%. A bone marrow biopsy was performed, which shows trilineage proliferation and pleiomorphic megakaryocytes. His prior medical history is notable for smoking. Based on a diagnosis of polycythemia vera, the patient is started initially on phlebotomy and aspirin.
Now, a few months later, the patient has undergone 3 phlebotomies, essentially monthly, and complains of continued dizziness, headaches, and nausea. At this time, he is continued on phlebotomy as needed and aspirin, but now hydroxyurea is added, a dose of 1,000 milligrams per day. A few months later, he’s had a couple more phlebotomies, and the dosage of hydroxyurea once again is increased now to 1500 milligrams per day.
Now it’s November, the patient is still dependent on phlebotomies and he also complains of itching. The dose of hydroxyurea is increased up to 2 grams per day. And in February, 1 year postdiagnosis, he’s had a couple more phlebotomies since November, he’s averaging about a phlebotomy per month, and he’s also experiencing abdominal fullness and some taste changes. His spleen is now palpable at 6 centimeters below the costal margin.
Overall, as a summary, this is a patient with polycythemia vera and over the course of a year, required phlebotomies on average once a month despite increasing doses of hydroxyurea. He also had some symptoms of moderate splenomegaly and itching, as well as headaches and some taste changes.
Transcript edited for clarity.